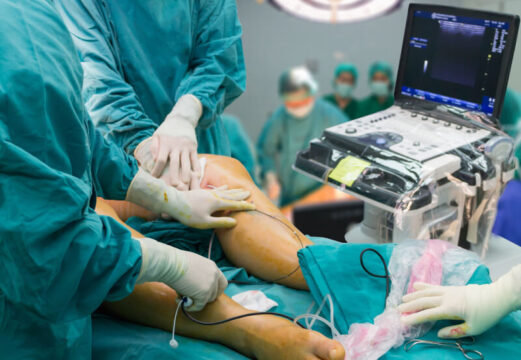
The study analyzed 642 patients undergoing TAVR. Patients were followed up with Doppler Echocardiography and, those presenting symptoms or gradient increase underwent CT and TEE.
Thrombosis was defined according to Latib criteria: 1) valve dysfunction: >20 mmHg gradient, <1.2 cm2 valve area reduction secondary to thrombosis diagnosed by imaging (TEE or CT); 2) suspicious mobile mass in the valve different from dysfunction or in absence of infection. It was considered acute within 10 days after TAVR; subacute, from 10 days to a month; or late after a month.
Thrombosis was found in 18 patients (2.8%), with no differences between the groups. 58.8% of patients received dual ATP at least 3 months, while 40,6% received oral anticoagulation plus clopidogrel.
Thrombosis presented at 181 days, mean gradient and area were 34±14 mmHg and 1±0.46 cm2. It was more frequent in expandable balloons (OR 3.45; 95% CI 1.22 to 9.81; p=0.01) and in V-in-V (OR 5.93; 95% CI 2.01 to 17.51; p=0.005) and it was associated with peptide natriuretic increase. In those receiving antiaggregation it was 4.8%, and it was not found in those receiving anticoagulation.
In patients treated with anticoagulation, symptoms improved, gradient was reduced, valve area increased and peptide natriuretic was reduced. There were no deaths associated to thrombosis.
Conclusion:
Post TAVR clinical thrombosis is more frequent than we used to think and it is characterized by abnormal imaging, and gradient and peptide natriuretic increase. This occurs more frequently in balloon expandable valves and V-in-V. Oral anticoagulation seems more effective in preventing valve thrombosis. The optimal antithrombotic therapy still calls for randomized studies.
Commentary
This retrospective analyzis shows thrombosis in the real world is more frequent than we thought. Therefore, we should watch closely for it at patient follow up.
We should enquire deeper during follow up, thoroughly interpret Doppler ECG findings, and act accordingly whenever we suspect of valve thrombosis.
The good news is it can be solve with anticoagulation and is not associated with mortality.
It is still unclear what group is at risk and how we should proceed. We need to continue our research and analyze whether it has a learning curve.
Courtesy of Dr. Carlos Fava
Original Title: Clinical Bioprosthetic Heart Valve Thrombosis after Transcatheter Aortic Valve Replacement. Incidence, Characteristics and Treatment Outcomes
Reference: John Jose, et al. J Am Coll Cardiol Intv 2017;10,686-97
Subscribe to our weekly newsletter
Get the latest scientific articles on interventional cardiology
We are interested in your opinion. Please, leave your comments, thoughts, questions, etc., below. They will be most welcome.