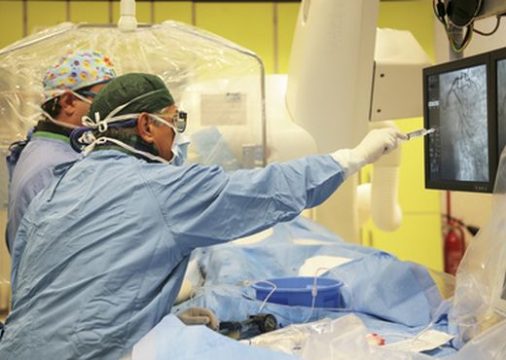
Is the Obesity Epidemic Putting Patients’ and Physicians’ Health at Risk?

Operators are clearly and increasingly exposed to radiation as patient body mass index (BMI) increases. Radiation exposure might be 7 times higher when treating ≥40 BMI patients, compared against <25 BMI patients, according to this study recently published in Circulation Cardiovascular Interventions.
Read also: Radiation Exposure in Chronic Total Occlusions.
Obesity has a negative impact on patients’ health and, since average BMI is on the rise (up to 85% of patients admitted to the cath lab is overweight or obese) occupational hazard is expected to rise accordingly. Scatter radiation emitted by patients is the highest source of radiation for operators and has direct correlation with patient radiation dose.
This was a prospective study (SHIELD study) in which operators working in two suites with identical fluoroscopy systems wore dosimeters to collect real-time radiation exposure data during 1,119 consecutive coronary angiography procedures. Patient radiation exposure was estimated using dose area product and air kerma.
The standard procedure included two protection shields between patient and operator. The use of disposable pads to cover patients and absorb radiation was left to operators’ discretion, and at least one of these was used in 59% of cases. The higher the BMI, the more often they were used.
Read also: Protective Shield RADPAD Reduces the Radiation Dose Received by Operators in the Cath Lab.
Average BMI was 30.8 kg/m², half of patients were obese, and 9.6% were morbidly obese.
Compared against <25 BMI, ≥40 BMI was associated with a two fold increase radiation dose according to either dose area product or air kerma, though physician exposure was proportionally higher, increasing from 0.2 to 1.4 µSv (P < 0.001 for all). This was observed in both diagnostic procedures and PCI.
In multivariable analysis, each 1-unit increase in patient BMI was independently associated with a 5.2% increase in physician radiation dose (P < 0.0001). Other factors associated with higher exposure were older age, PCI, and use of fractional flow reserve, whereas use of a radiation-absorbing pad was reduced physician exposure.
All this information comes out in the context of increasing evidence supporting the risks of operator radiation exposure, like early cataract, early carotid atherosclerosis, brain tumors on the left side, and acute DNA damage.
Original title: Patient body mass index and physician radiation dose during coronary angiography: is the obesity epidemic impacting the occupational risk of physicians in the catheterization laboratory?
Reference: Madder RD et al. Circ Cardiovasc Interv. 2019;12:e006823.
Subscribe to our weekly newsletter
Get the latest scientific articles on interventional cardiology
We are interested in your opinion. Please, leave your comments, thoughts, questions, etc., below. They will be most welcome.