Original Title: Effectiveness of Left Atrial Appendage Exclusion Procedures to Reduce the Risk of Stroke: A Systematic Review of the Evidence.
Reference: North Noelck et al. Circ Cardiovasc Qual Outcomes. July 2016. Published ahead of print.
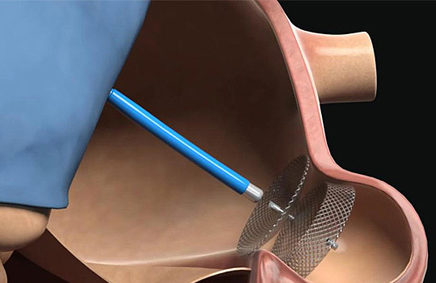 Atrial fibrillation is an important cause of stroke. Oral anticoagulation reduces the risk of stroke but, on the other hand, increases the risk of bleeding. Left atrial appendage closure procedures have been designed to isolate the left atrial appendage (LAA) from blood circulation and is an alternative to oral anticoagulation.
Atrial fibrillation is an important cause of stroke. Oral anticoagulation reduces the risk of stroke but, on the other hand, increases the risk of bleeding. Left atrial appendage closure procedures have been designed to isolate the left atrial appendage (LAA) from blood circulation and is an alternative to oral anticoagulation.
This study is a systematic review to assess the risks and benefits of percutaneous or surgical LAA closure.
In all, 20 studies met the pre-specified inclusion criteria, from where researchers recovered patient characteristics, and stroke, mortality and adverse events rates. The quality and state of evidence were also assessed according to publication criteria.
Researchers found studies with low quality evidence concluding LAA closure and anticoagulation had similar risk of stroke and mortality rates, noting, however, this evidence was limited to Watchman implantation in patients eligible for oral anticoagulation at short term.
Observational studies provide stronger evidence on the possibility of periprocedural adverse events after percutaneous LAA closure with practically all available devices.
There is little evidence on surgical LAA closure in the context of heart surgery for another indication (either cardiac or vascular), but it doesn’t seem to contribute to surgery-related adverse events that. There is insufficient data to argue that surgery will reduce stroke risk.
Conclusion
There is limited evidence to support the Watchman might be superior to long term oral anticoagulation in selected patients. There is not enough data on the effectiveness of different devices in patients who are ineligible for oral anticoagulation. Percutaneous LAA closure is associated with a relatively high risk of periprocedural complications.
We value your opinion. You are more than welcome to leave your comments, thoughts, questions or suggestions here below.





