The PRAGUE-17 has shown that left atrial appendage closure is not inferior to direct anticoagulants at long term to prevent major cardiovascular, neurological, or bleeding events. Moreover, procedures not related to prosthesis implantation saw significant reduction.
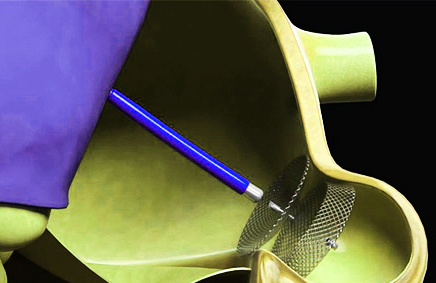
The PRAGUE-17 was a randomized non-inferiority study comparing left atrial appendage closure (Watchman or Amulet) with direct anticoagulants (95% received apixaban) in patients with non-valvular atrial fibrillation in addition to a history of cardio-embolism, clinically relevant bleeding or both (CHA2DS2-VASc ≥3).
Primary end point was a combination of cardioembolic events (stroke, transient ischemic attack, or systemic thromboembolism), cardiovascular death, clinically relevant bleeding, or procedure related complications (only for atrial appendage closure).
It included 201 patients in each group (mean age 73.3 ± 7.0). After 3.5 year mean follow-up, atrial appendage closure resulted non inferior to direct anticoagulants for primary end point.
Read also: PRAGUE-17: Appendage Closure vs. Direct Anticoagulant Agents.
Primary end point resulted similar for both for treatment intention and protocol analysis.
Conclusion
At long term followup, left atrial appendage closure resulted non inferior to direct anticoagulants in the prevention of cardiovascular, neurological, and bleeding events. After device implantation, bleeding saw significant reduction with these devices.
Original Title: 4-Year Outcomes After Left Atrial Appendage Closure Versus Nonwarfarin Oral Anticoagulation for Atrial Fibrillation.
Reference: Pavel Osmancik et al. J Am Coll Cardiol. 2022 Jan 4;79(1):1-14. doi: 10.1016/j.jacc.2021.10.023.
Subscribe to our weekly newsletter
Get the latest scientific articles on interventional cardiology





