Courtesy of Dr. Guillermo Migliaro.
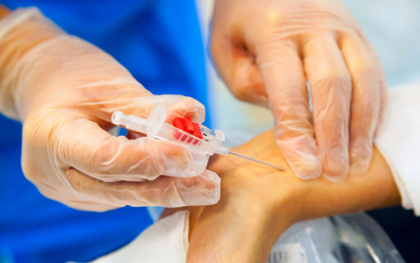 Coronary angiography and angioplasty via transradial approach are associated with a significant reduction in access site complications, compared with transfemoral and transbrachial access. Moreover, a significant reduction in mortality has been reported for procedures performed via transradial approach vs. transfemoral approach in primary angioplasty.
Coronary angiography and angioplasty via transradial approach are associated with a significant reduction in access site complications, compared with transfemoral and transbrachial access. Moreover, a significant reduction in mortality has been reported for procedures performed via transradial approach vs. transfemoral approach in primary angioplasty.
There is a limited number of studies comparing right and left transradial access. While right transradial access (RTA) is the preferred choice for most operators, it presents difficulties, mostly due to tortuosities in the subclavian artery, and reports suggest a higher incidence of stroke for this approach.
Left transradial access (LTA) does present a more direct pathway and is more similar to the transfemoral approach as regards catheterization, but is less convenient due to yuxtaposition at the abdomen.
This meta-analysis includes 12 randomized studies (5 diagnostic studies, and 7 therapeutic studies) comparing RTA and LTA in 6450 patients. There were no differences between groups regarding mean age and percentage of male patients.
Results
- The rates for failure or crossover were similar for both strategies: 4.2% for right transradial access and 4.1% for left transradial access (p = 0.68).
- The rates for procedure times were similar for both groups, 18.8 ± 10.3 min vs. 18.1 ± 10 min (p = 0.16).
- Right transradial access presented longer fluoroscopy time, 5.8 ± 4.4 min vs. 5.3 ± 4.2 min (p <0.001), and greater contrast use, 84 ± 35 mL vs. 82 ± 34 mL (p = 0.003), when compared with left transradial access.
- A subgroup analysis showed that these significant differences were present only in diagnostic studies, but not when therapeutic and diagnostic studies were analyzed jointly.
- There were no significant differences between both strategies regarding complications (0.6% for both groups) and the incidence of stroke (0.2% vs. 0.1%). There was a higher incidence of subclavian artery tortuosity in the right side (12% vs. 5%, p <0.0001).
Authors conclude that left transradial access is as safe and effective as right transradial access for both diagnostic and therapeutic procedures, with a small difference in fluoroscopy time and contrast use (for diagnostic procedures) in favor of the left radial approach.
Editorial
So far, this is the first comparative meta-analysis published comparing both strategies. This study does not report operator experience regarding access sites, which means that bias in this sense cannot be ruled out (some studies favor left transradial access for novice or training operators). The clinical relevance of the increase in fluoroscopy time for both patient and operator, and the relevance of the increase in contrast use for patients are still unclear.
Courtesy of Dr. Guillermo Migliaro. Buenos Aires German Hospital, Argentina.
Original title: Comparison of Transradial Coronary Procedures Via Right Versus Left Radial Artery Approach: A Meta Analysis.
Reference: Shah R et al. Catheter and Cardiovascular Interventions 2016;88:1027-1033.
Subscribe to our weekly newsletter
Get the latest scientific articles on interventional cardiology
We are interested in your opinion. Please, leave your comments, thoughts, questions, etc., below. They will be most welcome.





