Left atrial appendage occlusion (LAAO) is an alternative to prevent atrial fibrillation stroke mainly used in patients at high risk for bleeding.
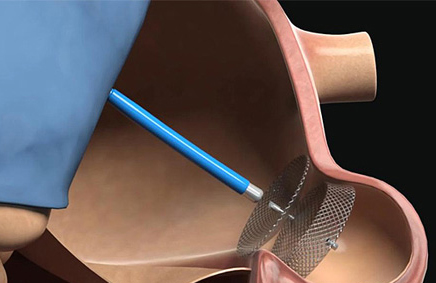
One of the most widely used devices in randomized trials is the Watchman, which yielded promising results. However, its real-life performance had yet to be analyzed.
Researchers conducted an analysis of the National Cardiovascular Data Registry of the American College of Cardiology, which includes 366,814 patients implanted with the Watchman device.
The primary endpoint (PEP) was ischemic stroke, while the secondary endpoint (SEP) included death, hemorrhagic stroke, undetermined stroke, intracranial bleeding, any stroke, systemic embolism, and major bleeding.
Mean age was 76 years old, 58% of the patients were male, patient BMI was 30 [sic], over 90% of patients were hypertensive, 38% had diabetes, 25% had a prior stroke, 14% had a prior TIA, and 18% had a history of thromboembolism.
The HAS-BLED score was 3 and the CHA2DS2-VASc score was 4.8; 70% of patients experienced major bleeding, 42% experienced digestive bleeding, and 12% experienced intracranial bleeding.
Atrial fibrillation was paroxysmal in 52% of cases; in all others, it was permanent or persistent.
Procedural success was 97%.
At discharge, 50% of patients received aspirin plus anticoagulation (warfarin or DOAC) and, to a lesser extent, anticoagulation or dual antiplatelet therapy.
Read also: Ticagrelor Shows Benefits in Coronary Microvascular Function after NSTEMI.
A one-year follow-up was conducted for 93.6% of patients.
The PEP was 1.53% (95% confidence interval: 1.39%-1.69%), the ischemic stroke rate was 2.19%, and all-cause mortality was 8.5%. The composite of stroke, systemic embolism, or death at a year was 10.7%. Major bleeding was 6.9% (mostly occurring within 45 days after discharge).
Conclusion
This study highlights the importance of the evolution of a cohort in the US with percutaneous closure of the left atrial appendage. Knowing the data, physicians and patients can make joint decisions on this therapy.

Dr. Carlos Fava.
Member of the editorial board of SOLACI.org .
Original Title: Clinical Outcomes at 1 Year Following Transcatheter Left Atrial Appendage Occlusion in the United States.
Reference: Matthew J. Price, et al. J Am Coll Cardiol Intv 2022;15:741–750.
Subscribe to our weekly newsletter
Get the latest scientific articles on interventional cardiology





