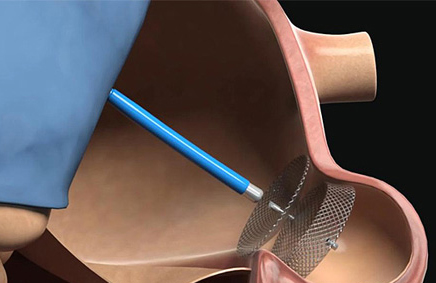
Percutaneous left atrial appendage closure (LAAO) with Watchman has FDA approval since March 2015, having shown, in the PROTECT-AF and PREVAIL studies, reduced risk of atrial fibrillation driven stroke, by excluding the left atrial appendage form systemic circulation.
Both studies used post procedure standardized protocols involving followup at 45 days and 6 months, imaging, and specific antithrombotic schemes. This is why the FDA issued their recommendations consisting of: antithrombotic treatment at discharge with warfarin and aspirin (80-325mg) for 45 days after implantation, transesophageal echocardiography at 45 days (first checkup) and in case of peri device leak >5mm, continuation of the same antithrombotic scheme. Without leak, continuation of dual antiplatelet therapy (DAPT) with clopidogrel for 6 months.
Real life patients present significant differences compared against those included in trials, especially when it comes to age and comorbidities (in addition to bleeding events). This is why, after device approval, they looked into LAAO patients in the National Cardiovascular Data Registry and assessed variations of the original treatment by the FDA, and protocol adherence.
The aim of this study was to assess deviation and different schemes used in real life patients through the NCDR registry, including patients from 2016 to 2018 treated with the first Watchman device.
Primary end point was any adverse event (neurological, pulmonary, cardiovascular or bleeding), major adverse events (death, cardiorespiratory arrest, AMI, significative pericardial effusion, systemic thromboembolism, stroke or major bleeding) stroke or transient ischemic attack (TIA) and/or readmission at 45 days. Secondary end point included the same events, only at 6 months.
Researchers analyzed data from 31994 patients, mean age 76, CHADS-VASC score of 4.6 and HAS-BLED=3. Only 12.2% followed every FDA approved recommendation (treatment and followup), the most common deviation being a different antithrombotic scheme to the one suggested, with warfarin and aspirin (61.5%). Post implantation strategies were warfarin and aspirin (36.9%), direct anticoagulant (DOAC) and aspirin (20.8%), warfarin alone (13.5%), DOAC alone (12.3%) and DAPT (5%).
The risk of any unadjusted adverse event was significantly higher in patients treated with warfarin and aspirin (5.7%) followed by DAPT (5.6%), mainly at the expense of bleeding events, with no difference in stroke or TIA. At regression analysis, the adjusted risk of any adverse event at 45 days was significantly lower with warfarin alone (HR: 0.658; CI 95% 0.536-0.808) and DOAC alone (HR: 0.767; CI 95% 0.597-0.985), vs. warfarin + aspirin.
Read also: Same Day Discharge in NSTE-ACS: Is It Possible?
The risk of any adverse event was significantly lower with warfarin (HR: 0.658; CI 95% 0.536-0.808) and DOAC (HR: 0.767; CI 95% 0.597-0.985), with no major risk of stroke, TIA or peri device leak >5mm.
At 6 months, there were fewer events in the warfarin group, with no risk of stroke or TIA.
Conclusions
In this registry, 70% of patients had some bleeding history, and average HAS-BLED in the population was 3. There was only 37% adherence to FDA recommended treatment of warfarin and aspirin. Also, the antithrombotic strategy of warfarin alone or DOAC alone showed fewer events, with similar incidence of stroke or TIA compared against warfarin + aspirin.
Please not this registry was not based on the Watchman FLX, but on the early version, unlike the PINNACLE FLX trial (DOAC + aspirin as antithrombotic).

Dr. Omar Tupayachi.
Member of the Editorial Board of SOLACI.org.
Original Title: Antithrombotic Therapy After Left Atrial Appendage Occlusion in Patients With Atrial Fibrillation
Source: Freeman JV, Higgins AY, Wang Y, Du C, Friedman DJ, Daimee UA, Minges KE, Pereira L, Goldsweig AM, Price MJ, Reddy VY, Gibson D, Doshi SK, Varosy PD, Masoudi FA, Curtis JP. Antithrombotic Therapy After Left Atrial Appendage Occlusion in Patients With Atrial Fibrillation. J Am Coll Cardiol. 2022 May 10;79(18):1785-1798. doi: 10.1016/j.jacc.2022.02.047.
Subscribe to our weekly newsletter
Get the latest scientific articles on interventional cardiology





