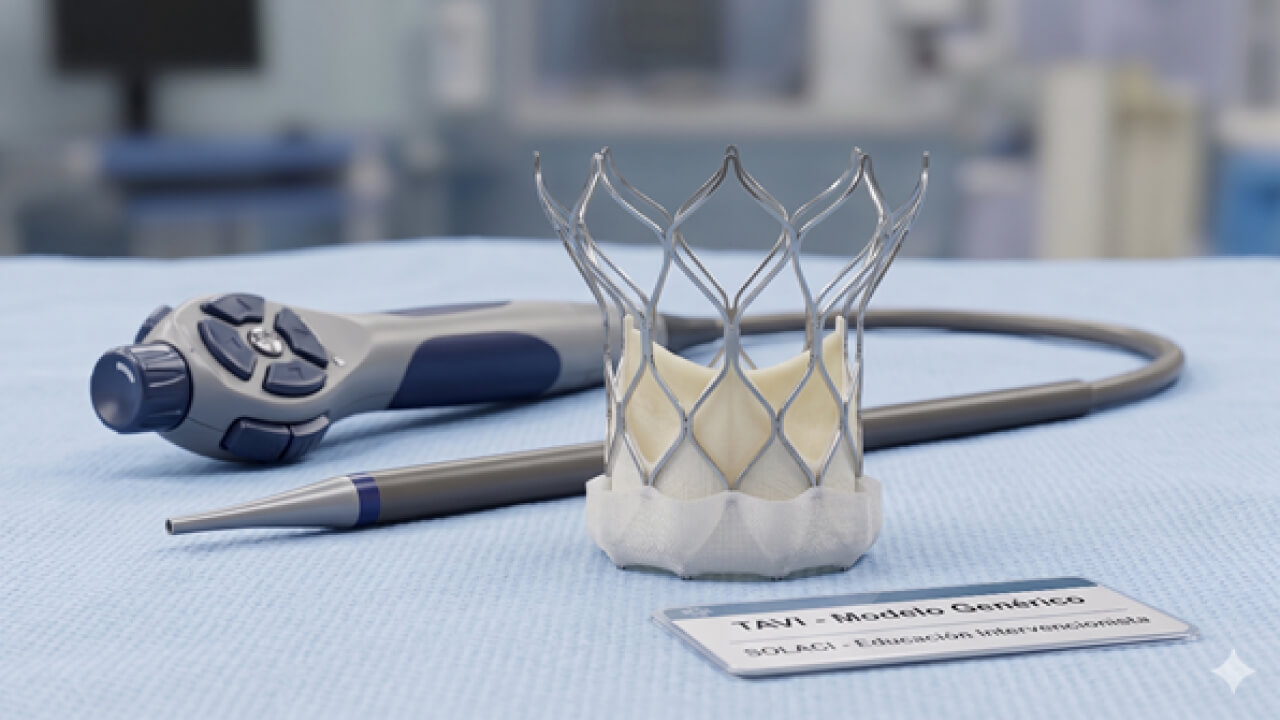
The expansion of TAVI, with the introduction of new-generation devices, has prioritized not only periprocedural safety, but also the preservation of coronary access, more favorable hemodynamics, and the reduction of paravalvular leak (PVL). The Navitor valve (Abbott) is an intra-annular, self-expanding transcatheter valve featuring inner and outer cuffs designed to reduce PVL. It also has an updated version (Navitor Vision) that incorporates radiopaque markers to optimize implantation depth.
The aim of this study was to describe early clinical and hemodynamic outcomes (primarily the composite of all-cause death or stroke at 30 days) in patients with native aortic stenosis treated with Navitor in real-world clinical practice (STS/ACC TVT registry). Patients who were candidates for valve-in-valve procedures and those with pure aortic regurgitation were excluded.
A total of 2,958 patients from 198 centers were included; the mean age was 81.4 years, 62.4% were women, and the STS-PROM was 6.6% ± 5.4%. Transfemoral access was used in 97.5% of cases, 73.6% were performed under conscious sedation, and the implanted valves were Navitor Classic in 75.6% and Navitor Vision in 24.4%.
Clinical outcomes and 30-day safety with the Navitor valve in real-world TAVI
The reported data showed a technical success rate of 97.9%, and in-hospital mortality was 1.3%. The mean procedure time was 58 minutes, with a mean length of stay of 1 day (93.7% discharged home).
Read also: Therapeutic strategies in carotid free-floating thrombus: evidence and controversies.
At 30 days, the composite of all-cause death or stroke was 5.2% (mortality 2.8%; stroke 2.7%). Major vascular complications occurred in 1.8% of cases, with 0.7% experiencing life-threatening or major bleeding. The rate of permanent pacemaker implantation (PPI) was 17.8% (14.1% in patients without baseline conduction disturbances). Among those requiring PPI, 42.8% had pre-existing conduction abnormalities.
In centers performing more than 20 implants per year, the PPI rate decreased significantly (from 19.4% to 13.5%, P = 0.0039 with the classic valve and from 19.1% to 10.6% with the Vision valve, P = 0.047).
In short-term follow-up, a mean transvalvular gradient of 7.3 mmHg was observed, with a low incidence of moderate or greater PVL (1.8%).
Conclusions: Hemodynamic performance and PVL reduction with Navitor and Navitor Vision
Original Title: Early U.S. Real-World Experience With a Novel Intra-Annular Self-Expanding Valve for Transcatheter Aortic Valve Replacement.
Reference: Garcia S, Sultan I, Rollefson W, Jones BM, Puri R, Krishnaswamy A, Tang GHL, Khera S, Gada H, Williams M, Shah AP, Talreja D, Yadav P, Thourani V. Early U.S. Real-World Experience With a Novel Intra-Annular Self-Expanding Valve for Transcatheter Aortic Valve Replacement. JACC Cardiovasc Interv. 2025 Dec 8:S1936-8798(25)02827-4. doi: 10.1016/j.jcin.2025.10.053. Epub ahead of print. PMID: 41518360.
Subscribe to our weekly newsletter
Get the latest scientific articles on interventional cardiology





