After four years of follow-up, the PRAGUE-17 study showed that appendage closure is non-inferior to direct anticoagulant agents (non-warfarin oral anticoagulants, NOAC) to prevent major neurological events, cardiovascular events, and bleeding events in patients at high risk of atrial fibrillation.
Appendage studies were compared with warfarin studies—it was necessary to update anticoagulant agents and reach a reasonable follow-up period.
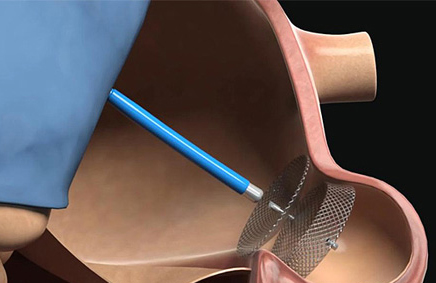
PRAGUE-17 randomized, with a non-inferiority criterion, patients who underwent appendage closure (Watchman or Amulet) vs. NOACs (apixaban in 95% of cases). These patients had experienced non-valvular atrial fibrillation and a history of cardioembolism, clinically relevant bleeding, or both (CHA2DS2-VASc > 3).
The primary endpoint was a composite of cardioembolic events (stroke, transient ischemic attack, or systemic embolism), cardiac death, clinically relevant bleeding, and device-related complications (only for the appendage closure group).
With 201 patients randomized to each group and after 3.5 years of median follow-up, appendage closure reached non-inferiority as regards the primary endpoint (pnon-inferiority = 0.0006)
Component rates (when considered separately) were similar, except for bleeding not related to the procedure. That was lower with closure devices. The bleeding risk is relevant during implantation; afterwards the risk lowers abruptly (as opposed to anticoagulant agents, with which the risk is ongoing).
Read also: CHOICE-CLOSURE | Which Closure Device for TAVR is Better?
Primary endpoint results are similar in the per protocol analysis and the per actual treatment analysis.
Conclusion
Long term follow-up of PRAGUE-17 showed that appendage closure with either of the two most popular devices is non-inferior to direct anticoagulant agents. Appendage closure devices were better in terms of bleeding not related to the procedure.
Original Title: Left Atrial Appendage Closure versus Non-Warfarin Oral Anticoagulation in Atrial Fibrillation: 4-Year Outcomes of PRAGUE-17.
Reference: Pavel Osmancik et al. J Am Coll Cardiol. 2021 Oct 27; S0735-1097(21)07895-5. Online ahead of print. doi: 10.1016/j.jacc.2021.10.023.
Subscribe to our weekly newsletter
Get the latest scientific articles on interventional cardiology





