Courtesy of Dr. Carlos Fava.
Surgical aortic valve replacement with bioprosthesis has proved its benefits, but it fails after 10 to 15 years.
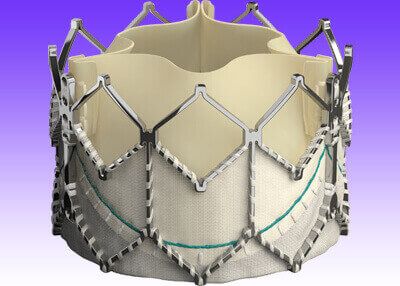
Transcatheter aortic valve replacement has been shown valid, especially in high risk patients, but we still have little information and no “head to head” studies to know what is best in this group that keeps growing over the years.
A retrospective analyzis of the National Readmissions Database (NRD) from 2012 to 2016 was carried out, including 6815 procedures, 3443 (50.5%) receiving V-in-V TAVI and 3372 re-SAVR.
The V-in-V TAVR group had older patients, with prior CABG, kidney function deterioration and cardiac failure.
At 30 days, this population had lower mortality (2.8% vs. 5.0%; OR 0.55, 95% CI 0.33 – 1.91), morbidity (66.4% vs. 79%; OR 0.52, 95% CI 0.41 – 0.66) and major bleeding (35.8% vs. 49.9%; OR 0.56, 95% CI 0.44 – 0.71). In addition, it presented shorter hospital stay (7 vs. 9 days, on average 2 days, 95% CI 1.4 – 2.6) and higher home discharge (45.9% vs. 34.2%; OR 1.57, 95% CI 1.28 – 1.93).
Read also: EuroPCR 2020 | Aortic Valve in Valve in the Long Term.
There were no differences in stroke, kidney failure, need for pacemaker, A-V block or cost between procedures. Likewise, there were no differences in rehospitalization need within 30 days.
On multivariable analyzis, the re-SAVR group was associated with higher mortality and morbidity and 30’ days.
When comparing groups, propensity score matching left 2181 pairs.
Read also: Is V-in-V the Treatment of Choice in Cases of Failed Biological Prosthesis?
At 30 day followup, V-in-V TAVR was associated to lower mortality (OR 0.41, 95% CI 0.23–0.74), lower morbidity (OR 0.53, 95% CI 0.43–0.72), lower major bleeding (OR 0.66, 95% CI 0.51–0.85), shorter hospital stay (on average two days 95% CI 1.3–2.7) and higher discharge (OR 2.11, 95% CI 1.61–2.78) compared against re-SAVR.
Patients undergoing re-SAVR had 59% more mortality, 63% morbidity and 71% major bleeding. Patients in the V-in-V TAVR group showed 3.9 more chances of home discharge compared against re-SAVR patients.
Conclusion
In this study of high-risk population with bioprosthetic aortic valve failure, V-in-V TAVR seems to have an advantage over re-SAVR at 30 days in terms of mortality, morbidity, and major bleeding.
Further study is necessary in low, intermediate, and high-risk patients to look into long term effectiveness.
Gentileza del Dr. Carlos Fava.
Original Title: Comparison of in-hospital outcomes and readmissions for valve-in-valve transcatheter aortic valve replacement vs. reoperative surgical aortic valve replacement: a contemporary assessment of real-world outcomes.
Reference: Sameer A. Hirji, et al. European Heart Journal (2020) 0, 1–9. doi:10.1093/eurheartj/ehaa252.
Get the latest scientific articles on interventional cardiologySubscribe to our weekly newsletter
We are interested in your opinion. Please, leave your comments, thoughts, questions, etc., below. They will be most welcome.





