Severely calcified coronary stenosis poses a significant challenge for coronary angioplasty procedures. Modifying plaque before stenting is crucial to a successful intervention, since it will prevent the sub expansion associated to worse clinical outcomes at followup. The tools employed to assess complex lesions include specialized balloons such as cutting, scoring, or high pressure balloons, as...
Dissection and Re-Entry Technique in Chronic Total Occlusions: Data from the PROGRESS-CTO Registry
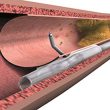
The antegrade dissection and re-entry (ADR) technique is considered essential for the management of chronic total occlusions (CTO). It serves as the primary option in some protocols for complex and extensive lesions or as a backup strategy in case of failure with other initial strategies. Dissection techniques include guided methods such as scratch and go,...
Retrograde Approach to Chronic Total Occlusions: Techniques and Outcomes According to the PROGRESS-CTO Registry
The retrograde approach for recanalizing chronic total occlusions (CTO) has undergone significant evolution since its introduction in 1990, improving both in terms of techniques and specialized materials. The increased skill applied to this strategy has resulted in increased success rates for the treatment of CTO in sites with an adequate volume of procedures. Given the...
Predictors of Stroke at 30 Days and 6 Months After TAVR
While the rate of stroke has decreased since the early days of transcatheter aortic valve replacement (TAVR), it remains non-negligible, reaching up to 1%-3% at 30 days. As TAVR progressively expands to low-risk populations and younger patients, identifying risk factors for patient selection and management in stroke prevention becomes crucial. While researchers have identified predictors...
ROTACUT Study: Rotational Atherectomy with Cutting Balloon for Stent Expansion Optimization
Approximately 30% of patients undergoing percutaneous coronary intervention (PCI) present moderate to severe calcified lesions, which presents a significant challenge involving a high incidence of major adverse cardiovascular events (MACE). Rotational atherectomy (RA) is used to modify these calcified lesions and facilitate balloon angioplasty followed by stent implantation. The combination of RA with other plaque...
Is Coronary Lithotripsy as Effective as Rotational Atherectomy?
Severely calcified lesions currently pose a significant challenge, as they require adequate preparation through non-compliant balloons or cutting balloons to achieve effective stent expansion. Another option is the use of orbital or rotational atherectomy (RA), but this carries the risk of complications such as slow/no reflow, perforations, dissections, peri-procedural infarction, or guidewire rupture. Despite the...
OBSERVANT II: Post TAVR 30-Day and 6-Month Stroke Predictors
Despite stroke rate has declined since the early days of transcatheter aortic valve replacement (TAVR), it remains significant, reaching 1% to 3% 30 days after procedure. Since TAVR has seen a progressive expansion to the low risk and young populations, identifying risk factors in patient selection and management is crucial for us to prevent stroke. ...
ROTA.shock Outcomes: Intravascular Lithotripsy vs. Rotational Atherectomy
At present, severe calcified coronary stenosis poses a significant challenge for PCI. A successful intervention will require plaque modification prior stenting, seeing as sub-expansion has been associated with worse clinical outcomes at followup. The tools normally used to treat these complex lesions include specialized balloons such as cutting, scoring, and high pressure balloons, as well...
Predictors and Evolution of Need for PPM after TAVR with Self-Expanding Valves
In the context of TAVR, one of the current challenges is the need for permanent pacemaker implantation (PPM), especially when using self-expanding valves (SEV). The information available in this regard remains controversial; while some studies suggest new PPM implantation will have no significant effect on clinical evolution, others have associated them with worse prognosis. As...
ESC 2023 | OCTOBER TRIAL: Should We Begin to Consider OCT for Bifurcation Lesions?
The OCTOBER Study randomized 1201 patients with bifurcation lesions in a 1:1 ratio to undergo percutaneous transluminal coronary angioplasty (PTCA) guided by optical coherence tomography (OCT) or by angiography. The primary endpoint (PEP) was major adverse cardiovascular events (MACE) over a 2-year period. Group characteristics were similar. The average patient age was 66 years, most...