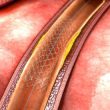
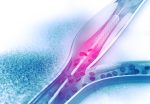
Follow-up of drug-coated balloon angioplasty in femoropopliteal disease in a real-world population. Using drug-releasing devices has decreased the rate of restenosis in obstructive femoropopliteal lesions compared with conventional balloons or conventional stents (bare-nitinol stent, BNS). Both in the placement of BNS and of drug-eluting stents (DES) there is a mechanical risk of stent fracture or...
BIODEGRADE: Does Stent Design Affect Long-Term Clinical Results?
Recent studies have shown that drug-eluting stents with biodegradable polymer and ultrathin struts are safe and effective, including low rates of stent thrombosis. This is why researchers conducted the BIODEGRADE (Biomatrix and Orsiro Drug-Eluting Stents in Angiographic Result in Patients With Coronary Artery Disease) study, which showed the non-inferiority at 18 months of ultrathin biodegradable polymer...
Intracoronary Brachytherapy for Drug-Eluting Stent Restenosis
3 Year Clinical Outcome Analysis and Failure Predictors in the Use of Intracoronary Brachytherapy for Drug-Eluting Stent Restenosis In-stent restenosis (ISR) has been one of the greatest obstacles standing in the way of long term patency in percutaneous coronary interventions. However, the use of drug eluting stents (DES) and their development has helped reduce ISR...
Plaque Erosion with No Stenting in Acute Coronary Syndrome: Are There Event Predictors to Avoid This Strategy?
Event predictors in patients with plaque erosion and no stenting. A third of all acute coronary syndrome (ACS) cases are caused by plaque erosion. In the initial EROSION study, it was shown that patients with plaque erosion (as evidenced by OCT, with stenosis <70%, TIMI III flow, and asymptomatic) were stabilized without stent implantation (no...
Stent Revascularization in Femoropopliteal Disease: An Analysis of Clustered Randomized Trials
A study compared pooled data of claudication and critical ischemia patients treated with stenting vs. by-pass surgery in femoropopliteal disease. The main objective of revascularization in femoropopliteal disease is to improve the quality of life and functional capacity of claudication patients who did not respond to medical treatment, and to save the affected limb in...
Can Drug Coated Balloon Be a Valid Option for Small Vessels?
One of the challenges of percutaneous coronary interventions (PCI) are <2.5 mm vessels, since complications and restenosis complications rate are higher than with >3.0 mm vessels. Drug Coated Balloons (DCB) can be a useful tool, but their efficacy and safety [vs. plain old balloon angioplasty] remains unclear. PEPCAD China SVD is a prospective and multicenter...
What Is the Best Strategy for Moderately Complex Femoropopliteal Lesions?
At present, PCI is the preferred treatment for femoropopliteal lesions and drug coated balloons (DCB) have shown good performance. However, they have not yet been shown superior to bare-metal stents (BMS). This study compared randomized trials IN.PACT SFA I/II and IN.PACT JAPAN including 288 patients vs. the prospective Complete SE and DURABILITY II with 483...
The Most Important Articles of 2022 in Peripheral Vascular Disease
Discover the most important scientific articles of 2022 in peripheral vascular disease in our website. EMINENT Trial | Stent Eluvia vs BMS in Femoropopliteal Territory Endovascular therapy in femoropopliteal territory has become the standard, mainly with self-expanding stents, aimed at preventing early vascular recoil and late constrictive remodeling. Thromboendarterectomy vs. Endovascular Therapy in Common Femoropopliteal...
Left Main Coronary Artery PCI Using State-of-the-Art Zotarolimus-Eluting Stents
Percutaneous coronary intervention (PCI) to the left main coronary artery (LMCA) with drug-eluting stent implantation is currently a major challenge due to the size of the vessel, the compromise of a bifurcation lesion in important branches, and the potential risk of complications. Available information on LMCA PCI comes from studies where DES stents were implanted...
Invasive Myocardial Viability Indexes
From a cellular standpoint, the term ‘myocardial viability’ refers to a myocyte that has no irreparable damage. From a clinical standpoint, it refers to areas with myocardial contractile dysfunction at rest that are expected to improve with correct revascularization. There are specific vessel ischemia and viability indexes that may help identify hibernation areas that could...