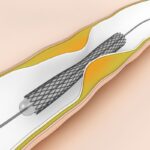
Original title: Heparin monotherapy or bivalirudin during percutaneous coronary intervention in patients with non-ST-segment elevation acute coronary syndromes or stable ischemic heart disease: results from the Evaluation of Drug-Eluting Stents and Ischemic Events registry. Reference: Bangalore S et al. CircCardiovascInterv. 2014;Epub ahead of print. Bivalirudin compared to unfractionated heparin as monotherapy is associated with a lower risk of<a href="https://solaci.org/en/2014/05/14/increased-security-with-bivalirudin-than-with-heparin-alone-in-patients-without-st-segment/" title="Read more" >...</a>
Angioplasty in sirolimus – eluting stent restenosis is safe and effective beyond the change of drug.
Original title: Sirolimius-eluting versus paclitaxel-eluting stents in diabetic and non-diabetic patients within sirolimus-eluting stents restenosis: Results from the ISAR-DESIRE 2 trial. Reference: Sebastian Kufner, et al. Cardiovascular Revascularization Medicine 2014, 15:69-75. DES restenosis has always generated a challenge and a puzzle when defining the strategy of revascularization by angioplasty: A quite used concept was to switch to<a href="https://solaci.org/en/2014/05/06/angioplasty-in-sirolimus-eluting-stent-restenosis-is-safe-and-effective-beyond-the-change-of-drug/" title="Read more" >...</a>
Coronary Artery Bypass Grafting and Percutaneous Coronary Intervention show similar outcomes for ostial/midshaft lesion in Unprotected Left Main Coronary Artery
Original title: Long-Term Clinical Outcome Intervention Versus Coronary Artery Bypass Grafting for Ostial/Midshaft Lesion in Unprotected Left main Coronary Artery From The DELTA Registry. Reference: Toru Nagamuna et al. JACC Cardiovascular Intervention. Article in Press Even though surgery remains the “gold standard” to treat UMCLA lesions, current guidelines have incorporated PCI as class IIa at ostium/midshaft level. The<a href="https://solaci.org/en/2014/04/04/coronary-artery-bypass-grafting-and-percutaneous-coronary-intervention-show-similar-outcomes-for-ostial-midshaft-lesion-in-unprotected-left-main-coronary-artery/" title="Read more" >...</a>
Deferred Stenting in Primary Angioplasty could reduce No Reflow Risk and Infarct Size.
Original: A Randomized Trial of Deferred Stenting versus Immediate Stenting to Prevent No-or Slow Reflow in Acute ST-Elevation Myocardial Infarction (DEFER-STEMI). Reference: David Carrick et al. J Am Coll Cardiol. 2014. Epub ahead of print. No Reflow physiopathology involves microvascular obstruction secondary to thrombus embolization, spasm or microvascular thrombosis, and happens in approximately 10% of PCI procedures. The<a href="https://solaci.org/en/2014/03/17/deferred-stenting-in-primary-angioplasty-could-reduce-no-reflow-risk-and-infarct-size/" title="Read more" >...</a>
Prophylactic vena cava filters in trauma patients effectively reduces pulmonary embolism
Original title: The effectiveness of prophylactic inferior vena cava filters in trauma patients: a systematic review and meta-analysis. Reference: Haut ER et al. JAMA Surg. 2014;149:194-202. Trauma is one of the strongest risk factors for pulmonary embolism (PE). Current guidelines recommend low molecular weight heparin therapy which have been proved effective; however, trauma patients often present high risk<a href="https://solaci.org/en/2014/03/12/prophylactic-vena-cava-filters-in-trauma-patients-effectively-reduces-pulmonary-embolism/" title="Read more" >...</a>
Best results of angioplasty with DES guided by IVUS versus angiography only
Original title: Intravascular Ultrasound-Guided Implantation of Drug-Eluting Stents to Improve Outcome. A Meta-Analysis. Reference: Jae-Sik Jang et al. J Am Coll Cardiol Intv 2014, epub ahead of print. Several previous studies and meta-analysis showed that implantation of conventional stents (BMS) intravascular ultrasound (IVUS) guided may decrease restenosis and clinical events. This information was not yet clear to drug-eluting<a href="https://solaci.org/en/2014/02/26/best-results-of-angioplasty-with-des-guided-by-ivus-versus-angiography-only/" title="Read more" >...</a>
At least one month of antiplatelet seems sufficient after a zotarolimus -eluting stent
Original title: Lack of association between dual antiplatelet therapy use and stent thrombosis between 1 and 12 months following Resolute zotarolimus-eluting stent implantation. Reference: Silber S, Kirtane AJ, Belardi JA, et al. Eur Heart J. 2014; Epub ahead of print. Dual antiplatelet aggregation optimal time after implantation of a new generation drug-eluting stent (DES) is still discussed. This<a href="https://solaci.org/en/2014/02/25/at-least-one-month-of-antiplatelet-seems-sufficient-after-a-zotarolimus-eluting-stent/" title="Read more" >...</a>
The length of the stent is not an event predictor with the new generation of DES. It is the end of the Spot stenting?
Original title: Impact of the Stent Length on Long-Term Clinical Outcomes Following Newer-Generation Drug-Eluting Stent Implantation. Reference: Ik Jun Choi et al. Am J Cardiol 2014;113:457-464. Completely cover the lesion with a sufficiently long stent has been the preferred strategy that emerged from drug-eluting stents (DES). However, for the first-generation DES stent length has been a predictor of<a href="https://solaci.org/en/2014/02/20/the-length-of-the-stent-is-not-an-event-predictor-with-the-new-generation-of-des-it-is-the-end-of-the-spot-stenting/" title="Read more" >...</a>
3rd generation zotarolimus-eluting stent non- inferior to everolimus
Original title: Third-generation zotarolimus-eluting and everolimus-eluting stents in all-comer patients requiring a percutaneous coronary intervention (DUTCH PEERS): a randomized, single-blind, multicentre, non-inferiority trial. Reference: Von Birgelen C et al. The Lancet. 2014; Epub ahead of print. In the 3rd generation zotarolimus-eluting stent, platform was modified to increase flexibility and make implant easier in complex lesions. This study was<a href="https://solaci.org/en/2014/02/13/3rd-generation-zotarolimus-eluting-stent-non-inferior-to-everolimus/" title="Read more" >...</a>
Almost 40 % of those who initially receive clopidogrel then switch to prasugrel or ticagrelor in clinical practice.
Original title: In-hospital switching of oral P2Y12 inhibitor treatment in patients with acute coronary syndrome undergoing percutaneous coronary intervention: Prevalence, predictors and short-term outcome. Reference: Dimitrios Alexopoulos et al. Am Heart J 2014;167:68-76.e2. Given the availability of 3 Oral P2Y12 receptor inhibitors (clopidogrel, prasugrel, and ticagrelor) with different safety and efficacy profiles, the change from one to another<a href="https://solaci.org/en/2014/02/07/almost-40-of-those-who-initially-receive-clopidogrel-then-switch-to-prasugrel-or-ticagrelor-in-clinical-practice/" title="Read more" >...</a>