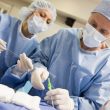
There are increasingly more patients who have undergone transcatheter aortic valve replacement (TAVR) and require a non-cardiac intervention, or patients with other diseases who need surgery and are diagnosed with aortic stenosis. In addition, on many occasions, surgery must be performed as soon as possible (as in cases of cancer) or is an emergency procedure....
More Screening Needed Before Non-Cardiac Surgery
According to this recent document by the American Heart Association (AHA), troponin should be monitored for at least 3 days after surgery. With about 20% of patients (most of them, asymptomatic) showing elevated troponin after a non-cardiac surgery, this new AHA document recommends monitoring, for at least two days, patients with moderate to severe ischemia. Myocardial...
How to Discontinue Antiplatelet Therapy Prior Non-Cardiac Surgery
Both the indication and discontinuation of antiplatelet therapy to balance ischemic-bleeding risks has been left to physician criterion. However, leaving the decision to one single specialist might not be the best. This is when the team’s role becomes essential. This study looked at the advantages consensus decision-making amongst clinicians, surgeons and anesthesiologists to continue or...
Discharge During the Weekend After Cardiac Surgery Is Not Associated with Readmissions
According to this new work (soon to be published in Ann Thorac Surg), discharging a patient during the weekend or a holiday after cardiac surgery is not associated with higher rates of readmission compared with patients discharged during weekdays. A total of 4877 patients were discharged after cardiac surgery in high-volume sites in the United States. Among them,...
Is Emergency Cardiac Surgery Necessary in TAVR?
Life-threatening complications that require surgery during TAVR are infrequent. The proportion was originally thought to be between 1% and 2%. However, we now know that it is lower, even though we do not know how frequent it is or what are its most common causes. Its evolution, both in the short and in the long...
Aspirin During Noncardiac Surgery: Only in Patients with Prior Angioplasty
A new analysis from the POISE-2 study suggests that aspirin should not be withheld prior to noncardiac surgery in patients with a history of coronary angioplasty, even if their coronary procedure occurred several years earlier. Patients with a history of coronary angioplasty who need cardiac surgery are more likely to benefit from continued aspirin therapy,...
TRICS III: Restrictive Transfusion Was Noninferior to Liberal Use in Patients Who Undergo Cardiac Surgery
A large study conducted in 19 countries has found that a policy of restrictive red-cell transfusion during cardiac surgery is just as safe and effective as more liberal policies. TRICS III enrolled 5243 patients and was presented at the American Heart Association (AHA) Scientific Sessions and published simultaneously in the New England Journal of Medicine (NEJM). Patients were...
Closing off the Appendage While Performing Cardiac Surgery Results in a Reduction in Risk of Embolic Stroke
Closing off the left appendage as an add-on procedure while performing other cardiac surgery in patients with atrial fibrillation resulted in a reduction in risk of embolic stroke of nearly 40% over 12 months, according to an analysis carried out on the Society of Thoracic Surgeons (STS) database. Patients who had surgical appendage occlusion had...
Incomplete Revascularization: Increased Events Rate in Non-Cardiac Surgery?
The aim of this study was to determine whether incomplete revascularization is associated to higher adverse events risk and acute myocardial infarction in patients undergoing non-cardiac surgery. Coronary artery disease patients or patients with prior PCI often have non cardiac surgery. These patients may have had all obstructions treated before surgery (complete revascularization) or...
Non-Cardiac Surgery with Incomplete Revascularization, Associated to Events
This study presented at the American Heart Association Scientific Sessions 2016 and simultaneously published in the Journal of the American College of Cardiology, showed incomplete revascularization is associated with an increased risk of adverse cardiac events, particularly infarction, in patients that must later receive non-cardiac surgery. Patients with incomplete revascularization (defined as a ≥ 50% left...