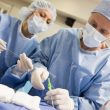
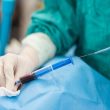
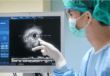
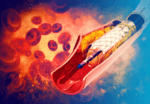
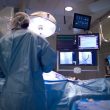
Transcatheter aortic valve replacement (TAVR) has widely demonstrated its significant benefits, both in high-risk and inoperable patients, as well as in those with intermediate and low risk. While paravalvular regurgitation has been a challenge, its management has improved with operator experience and a deeper understanding of CT angiographies. However, in cases of regurgitation, elevated gradient,...
Coronary Artery Disease in TAVR: Unsolved Dilemma
Aortic stenosis shares risk factors with coronary artery disease (CAD), and its prevalence varies according to age, reaching approximately 50% or more in some registries. Deciding when to treat and the need for percutaneous intervention presents a challenge. It has been established that epicardial stenosis at proximal level, or the medial segment, requires intervention, especially...
Transcatheter Mitral Valve Replacement: DOAC or VKA?
Severe mitral disease is common and currently constitutes a frequent cause of hospitalization and death. While surgery is the treatment of choice, transcatheter mitral valve replacement (TMVR) emerges as a valid alternative in cases of bioprosthesis failure, ring malfunction, or severe mitral annular calcification (MAC). Furthermore, the latest medical guidelines support the recommendation of TMVR...
Intramural Hematoma
Intramural hematoma (IMH) is considered a subtype of acute aortic syndrome (AAS), and some authors describe it as a developmental stage that might cause high morbimortality events such as dissection, aneurysm, or aortic rupture. One of the CT findings associated with IMH is focal contrast enhancement (FCE) within the intramural hematoma, with a reported incidence...
Relationship of Radial Wall Strain with Functional and Morphological Assessment of Coronary Artery Lesions
Radial wall strain (RWS) has been recently linked with plaque vulnerability and has been identified as a predictor of lesion progression and clinical outcomes. However, RWS should be assessed together with physiological indices and plaque characteristics. The aim of this post hoc analysis of the CCTA-FFR registry was to look into the link between RWS...
Use of IVUS in Complex PCI: Results according to Operator Experience
The use of ultravascular ultrasound (IVUS) to guide coronary angioplasty procedures (PCI) has been shown to reduce the risk of major adverse events in numerous randomized controlled studies, registries and meta-analysis. The current guidelines recommend the use of IVUS in left main disease and complex lesions. The proportion of complex PCI procedures has increased over...
iFR Guided PCI to the LAD: Same as for non-LAD Vessels?
iFR has been validated as a useful tool for intermediate lesion analysis, with the advantage of not requiring the use of drugs. On the other hand, its use for PCI outcome assessment has not yet been thoroughly looked into, even though there have been promising data. 24% of DEFINE PCI cases presented ≤0.89 iFR with...
Revascularization vs. Deferral of Physiologically Significant Lesions in the Left Main Coronary Artery
Most randomized studies on decision-making in coronary artery disease revascularization exclude left main coronary artery disease (LMCAD), as did the ISCHEMIA Study. On the other hand, the benefits of functionally assessing lesions, proven in studies such as FAME, emphasize the importance of this tool in guiding revascularization decisions. However, there is still little understanding of...
Cilostazol in Diabetic Patients with Endovascular Peripheral Revascularization: One Step Beyond Symptom Improvement
In patients with peripheral vascular disease (PVD), the presence of diabetes has been significantly associated with increased failure of critical lower limb ischemia (CLI) treatment, and higher incidence of amputation. This relationship has been attributed mainly to comorbidities and patient characteristics, concomitant peripheral neuropathy and marked microvascular alteration. Also, a high proportion of these patients...
Is Coronary Lithotripsy as Effective as Rotational Atherectomy?
Severely calcified lesions currently pose a significant challenge, as they require adequate preparation through non-compliant balloons or cutting balloons to achieve effective stent expansion. Another option is the use of orbital or rotational atherectomy (RA), but this carries the risk of complications such as slow/no reflow, perforations, dissections, peri-procedural infarction, or guidewire rupture. Despite the...