Angina persistence or recurrence after PCI can affect between 20 to 40% of patients in the short and mid-term. This might be true despite PCI optimization using FFR, intravascular ultrasound and the latest generation stents. This problem is associated with high healthcare cost, which can double in patients with recurrent or persistent angina compared against asymptomatic patients. Guidelines are unclear as to what to do; there are several gaps when it comes to their underlying physiopathological mechanisms, which makes these patients a real pain in the neck for clinical cardiologists and interventionists.
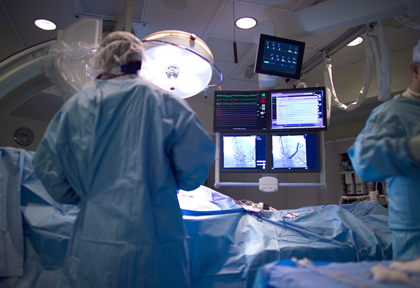
In the ORBITA trial, PCI benefits compared against a sham procedure resulted unclear. One of the potential mechanisms identified by the authors was microvascular angina, though this study has been criticized for having several methodological limitations.
Stent thrombosis and restenosis are infrequent cause of post PCI recurrent angina. In fact, in the contemporary daily practice, stent thrombosis rate is <1% during the first year and between 0.2 and 0.4% per year later on. Clinically relevant restenosis only explains 5% of patients at one-year follow-up.
Incomplete revascularization can occur in up to 30% of patients, though incomplete revascularization definitions are quite heterogeneous.
Read also: FDA Expands TAVR Indication to Low-Risk Patients.
Other potential causes of angina include diffuse atherosclerosis with no focal stenosis leading to persistent drop in blood pressure across the coronary tree.
Microvascular dysfunction might be another cause of post PCI angina. Indeed, stent implantation might cause or worsen this problem. This mechanism can be responsible in up to half the patients that still present symptoms, though it requires further prospective studies, as all other probable causes.
Chronic microcirculation adaptation to distal pressure reduction due to stenosis or epicardial occlusion could negatively affect its capacity to adapt to maximal dilation after flow and normal perfusion pressure restauration. Whatsmore, the capacity of microcirculation to recuperate normal vasomotor tone might vary in each patient.
PCI might also contribute to microvascular malfunction because of detritus microembolization that can occlude small arteries and/or capillaries. In addition, DES might cause vasoconstriction in the adjacent area, both in macro and microcirculation due to drug and polymer release.
Read also: Can Antiplatelet Therapy Affect the Life of Coronary Grafts?
Endothelial dysfunction might be prior, and it could actually be unmasked when sorting out the epicardial obstruction by PCI. Especially this kind of microcirculation dysfunction is implied in cardiac failure with conserved ejection fraction.
Last but not least, microcirculation regulates myocardial flow and therefore shear stress in the large epicardial vessels that might lead to vessel remodeling and plaque formation.
ESC guidelines for patients with stable coronary heart disease recommend a stress test at follow-up in patients with persistent or recurrent angina post PCI, preferably combined with imaging (class I, evidence level C). This way, a stress test in most cases represents the first diagnostic test for patients with post PCI angina.
Invasive studies in these patients are reserved for those with >10% myocardial ischemia (class I, evidence level C). However, we should burn stages and directly resort to a coronary angiogram in case of high-risk PCI (Class IIb, evidence level C).
Read also: FFR to Predict CABG Result: All Benefits in a Population Much Too Pure?
A few subtle data that might help in a differential diagnosis is that vasospastic angina usually happens at rest, often at night and with conserved tolerance to exercise. On the other hand, microvascular angina produces prolonged pain that does not respond immediately to nitrites.
Original Title: Mechanisms and diagnostic evaluation of persistent or recurrent angina following percutaneous coronary revascularization. On behalf of the Coronary Vasomotion Disorders International Study Group (COVADIS)
Reference: Filippo Crea et al. European Heart Journal (2019) 0, 1–10. Article in press.
Subscribe to our weekly newsletter
Get the latest scientific articles on interventional cardiology
We are interested in your opinion. Please, leave your comments, thoughts, questions, etc., below. They will be most welcome.





