Florencia Rolandi.2012-06-08
Antiplatelet Treatment with Ticagrelor vs. Clopidogrel in Patients with Chronic Coronary Syndrome
Achieving rapid and maximum inhibition of platelet aggregation can reduce complications related to scheduled percutaneous coronary intervention (PCI) in chronic coronary syndromes (CCS). Over the last few decades, the optimal timing for initiating P2Y12 inhibitors and their appropriate dosage have been the subject of numerous studies; however, they have not been clearly established yet. Higher...
ESC 2021 | MASTER DAPT: Dual Antiplatelet Therapy After Coronary Angioplasty in Patients at High Bleeding Risk
Courtesy of Dr. José Álvarez. In patients at high bleeding risk with drug-eluting stents, the duration of dual antiplatelet therapy has been subjected to ongoing review. Guidelines from the European Society of Cardiology (ESC) and the American College of Cardiology (ACC) suggest shortening this treatment to a maximum of three to six months (Class IIb)....
DAPT vs. Monotherapy: The Dilemma Remains After Surgery
Patients who undergo myocardial revascularization surgery and are discharged on dual antiplatelet therapy (DAPT)—aspirin plus clopidogrel—have a lower risk of major cardiovascular and cerebral events than patients on aspirin monotherapy. Furthermore, the risk of bleeding is not increased for those receiving DAPT. This information comes from a registry of over 18,000 patients recently published in the...
Dual Antiplatelet Therapy and TAVR: Obsolete Guidelines
The current guidelines recommend dual antiplatelet therapy (DAPT) 3 to 6 months after transcatheter aortic valve replacement (TAVI). Some recent data finally condensed in the present meta-analysis and recently published in JAHA happen to challenge these guidelines. Clinical studies that investigated single antiplatelet therapy versus DAPT until November 2020 were analyzed and divided according to...
We Should Indicate More than 6 Months of DAPT in Lower Limb Disease
Courtesy of Dr. Carlos Fava. Advanced peripheral vascular disease is frequently associated with cardiovascular events and amputation. It has been proven that mono-antiplatelet therapy (MAPT) offers some benefit (with either aspirin or clopidogrel), but there are scarce data on the role of dual antiplatelet therapy (DAPT) in these patients. Researchers analyzed 404 patients who received MAPT for...
Antiaggregation Time after Treating Bifurcations
Defining dual antiplatelet therapy (DAPT) seems a never-ending story. We go from trials showing the safety of shorter schemes thanks to new generation stents to others suggesting up to two years of DAPT. Rather than finding a general scheme, it seems to be about adjusting DAPT on a case by case basis, according to ischemia...
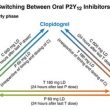
When and How to Switch Dual Antiplatelet Therapies
Dual antiplatelet therapy with aspirin and a P2Y12 inhibitor is the treatment of choice for patients with acute coronary syndrome who undergo coronary angioplasty. Different oral P2Y12 inhibitors (clopidogrel, prasugrel, ticagrelor) present different characteristics as regards efficacy, risk for bleeding, cost, and timing of administration. In this sense, physicians frequently switch among drugs according to...
Single or Dual Antiplatelet Therapy in Stroke or Transient Ischemic Attack?
Antiplatelet therapy is key to prevent thrombotic events after a transient ischemic attack (TIA) or ischemic stroke. The role of aspirin is well established in this scenario, but there is emerging evidence for a short period of dual antiplatelet therapy (DAPT). Now, can this strategy avoid recurrent strokes without paying a price in terms of...
Optimal Intervention Timing for NSTEMI with No Antiaggregant Pre-Treatment
Patients undergoing non-ST elevation MI (NSTEMI) who are not pre-treated with P2Y12 receptor inhibitors will benefit from a very early intervention strategy. The optimal intervention timing for NSTEMI patients is still under debate, despite multiple studies, but the ideal timing had never been tested in patients with no platelet aggregation inhibitor pretreatment. After the surge of...
- 1
- 2