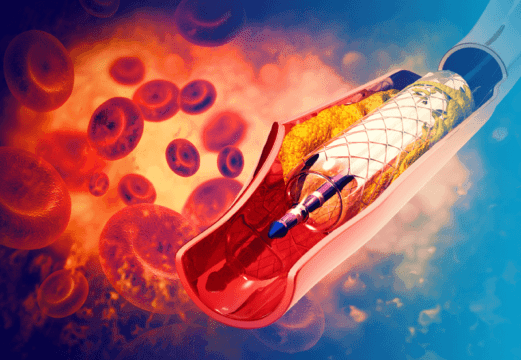
iFR has been validated as a useful tool for intermediate lesion analysis, with the advantage of not requiring the use of drugs. On the other hand, its use for PCI outcome assessment has not yet been thoroughly looked into, even though there have been promising data. 24% of DEFINE PCI cases presented ≤0.89 iFR with…
We Should Revascularize Patients with Stable Coronary Syndromes and Ischemia Assessed by iFR
Chronic stable angina has shown a good response to medical treatment, and the Ischemia study has recently demonstrated the safety of such treatment in stable chronic angina with moderate to severe ischemia. However, this study excluded left main coronary artery (LMCA) lesions. The FAME Study has shown the safety and efficacy of fractional flow reserve…
The Best of the SOLACI-SOCIME 2022 Main Arena: Day 3
Lecture by Dr. Hector García García – LM-PCI: IVUS and FFR/IFR? Dr. Hector García delivered an excellent presentation on whether we should use intravascular ultrasound (IVUS) or fractional flow reserve (FFR)/instantaneous wave-free ratio (iFR) in the left main coronary artery (LMCA) to consider severe obstruction, since there is significant interobserver variability with angiography. Although the…
Coronary Physiology Is Useful in Chronic Kidney Disease
Coronary physiology, FFR and iFR, has been shown safe to defer lesions and effective to save stents by different randomized studies and registries. However, patients with chronic kidney disease have not been thoroughly analyzed yet, which brings us to the question about what to do in the face of their negative evolution, when atherosclerosis develops…
FFR and IFR: Are We Talking About the Same Thing?
To evaluate borderline coronary lesions (a 40% to 70% obstruction), determining associated ischemia is paramount. For this purpose, pressure gradients are measured across the stenosis. These measurements can be hyperemic, such as the fractional flow reserve (FFR), or taken at rest, such as the instantaneous wave-free ratio (iFR). According to the iFR-SWEDEHEART 5-year follow-up outcomes,…
Coronary Angioplasty Evolution According to Syntax II: 5-Year Followup
It has been long since the SYNTAX (NEJM 2009) came out comparing percutaneous coronary intervention (PCI) against coronary artery bypass grafting (CABG). That emblematic study associated PCI with first generation drug eluting stents (Taxus) with increased major cardiac and cerebrovascular events (all-cause mortality, AMI, stroke, or any revascularization – MACCE) vs. CABG, at 5 years,…
Is iFR Reliable After 5 Years? Analyzing the iFR-SWEDEHEART at 5 Years
Fractional flow reserve (FFR) proved to be very useful and safe in the FAME study, but its trade-off was using adenosine (which has a short half-life) and adverse reactions, which fortunately were rare. Subsequently, two large studies—the iFR-SWEDEHEART and DEFINE-FLAIR—demonstrated that instantaneous wave-free ratio (iFR) offered comparable results to FFR in the short term, avoiding…
TCT 2021 | FAVOR III: Angiography-Derived FFR: An Event-Prevention Tool
Compared with visual estimation of lesions, using quantitative angiography-derived fractional flow reserve (quantitative flow ration, QFR) provides better clinical outcomes at one year for angioplasty. These results emerge from the Chinese FAVOR III study, presented at the 2021 TCT scientific sessions and simultaneously published in The Lancet. The simplicity and safety offered by QRF—since there is…
TCT 2021 | iFR-SWEDEHEART: 5 Years to Trust FFR Is Equivalent to iFR
The 5-year followup of the iFR-SWEDEHEART has confirmed the safety and efficacy of using either FFR or iFR to guide PCI in intermediate lesions. The iFR-SWEDEHEART initial outcomes together with the DEFINE-FLAIR outcomes had started the debate around these two measuring strategies. The FFR requires adenosine, which results costly in addition to causing adverse events,…
Large Differences between Focal and Diffuse Patterns of Stable CAD
PCI is far more successful at reducing ischemia when treating focal stable coronary artery disease (CAD). However, there were no differences in symptoms between both types of CAD. Physiological assessment with pressure wire pullback can be used to distinguish focal vs diffuse CAD, even though the relevance of this distinction has not been looked at…