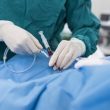
Abbreviated dual antiplatelet therapy in patients at high risk for bleeding and acute myocardial infarction. Patients with acute coronary syndrome (ACS) who undergo stent placement (percutaneous coronary intervention, PCI) conventionally require at least 12 months of dual antiplatelet therapy (DAPT) to reduce ischemic events. Patients with ACS who are also at high risk for bleeding<a href="https://solaci.org/en/2023/06/01/abbreviated-therapy-in-patients-with-acute-coronary-syndrome-how-safe-is-conservative-dapt-treatment/" title="Read more" >...</a>
Rivaroxaban in Acute Coronary Syndrome
Acute coronary syndromes (ACS) involve high mortality risk, especially ST elevation ACS. Their treatment is based on reperfusion, dual antiplatelet therapy (DAPT) and anticoagulation, with enoxaparin (1 mg/kg twice a day) as the preferred anticoagulant according to the contemporary guidelines. 2.5 mg or 5 mg doses of rivaroxaban might be valid alternative treatments for this<a href="https://solaci.org/en/2023/02/23/rivaroxaban-in-acute-coronary-syndrome/" title="Read more" >...</a>
Plaque Erosion with No Stenting in Acute Coronary Syndrome: Are There Event Predictors to Avoid This Strategy?
Event predictors in patients with plaque erosion and no stenting. A third of all acute coronary syndrome (ACS) cases are caused by plaque erosion. In the initial EROSION study, it was shown that patients with plaque erosion (as evidenced by OCT, with stenosis <70%, TIMI III flow, and asymptomatic) were stabilized without stent implantation (no<a href="https://solaci.org/en/2023/02/13/plaque-erosion-with-no-stenting-in-acute-coronary-syndrome-are-there-event-predictors-to-avoid-this-strategy/" title="Read more" >...</a>
Can We Use DAPT for 3 Months in Acute Coronary Syndrome?
Current guidelines recommend 12-month dual antiplatelet therapy (DAPT) after DES stenting for acute coronary syndrome (ACS) because of elevated MACE risk. The development of more modern stents, with thin and ultrathin struts, compared against prior versions, has resulted in more effective devices in terms of stent thrombosis and restenosis. Prolonged DAPT has been associated with<a href="https://solaci.org/en/2023/01/12/can-we-use-dapt-for-3-months-in-acute-coronary-syndrome/" title="Read more" >...</a>
RIPCORD 2 Study: Routine Assessment Using Pressure Wires in Acute Coronary Syndrome
The inclusion of fractional flow reserve (FFR) has changed how coronary interventions are treated. Current guidelines endorse its use in intermediate lesions with no evidence of ischemia in non-invasive studies in patients with multivessel disease. The original RIPCORD (Routine Pressure Wire Assessment Influence Management Strategy at Coronary Angiography for Diagnosis of Chest Pain) study proposed<a href="https://solaci.org/en/2022/09/12/ripcord-2-study-routine-assessment-using-pressure-wires-in-acute-coronary-syndrome/" title="Read more" >...</a>
Adherence to P2Y12 Inhibitors in Acute Coronary Syndrome: Prognosis
Non-adherence to medication in patients with acute coronary syndrome (ACS) remains to be solved; the use of polypills and a closer follow up have been tried out (follow up calls and motivation groups). Antiaggregation guidelines recommend dual antiplatelet therapy (DAPT) for at least one year after ACS. Adherence to drug treatment is comprised of multiple<a href="https://solaci.org/en/2022/08/30/adherence-to-p2y12-inhibitors-in-acute-coronary-syndrome-prognosis/" title="Read more" >...</a>
Aspiration Thrombectomy in Acute Coronary Syndrome: Is the Japanese Perspective a Strategy to Emulate?
Aspiration thrombectomy (AT) in patients with high thrombotic burden could pathophysiologically reduce thrombus burden, decrease distal embolization, reduce no-reflow phenomenon, and improve microvascular perfusion. However, its usefulness has not been shown in the large, randomized trials (TASTE and TOTAL) that compared routine use of AT in primary angioplasty in patients with ST-segment elevation acute coronary<a href="https://solaci.org/en/2022/08/26/aspiration-thrombectomy-in-acute-coronary-syndrome-is-the-japanese-perspective-a-strategy-to-emulate/" title="Read more" >...</a>
Prophylactic Rivaroxaban Therapy for Left Ventricular Thrombus after ST-Segment Elevation Acute Coronary Syndrome
The incidence of left ventricular thrombosis (LVT) after anterior ST-segment elevation myocardial infarction (STEMI) ranges from 4% to 26%. This is associated with bad long-term evolution. In the past, triple-scheme therapy (vitamin K antagonist plus dual antiplatelet therapy) was recommended to prevent LVT, despite the lack of high-quality scientific evidence and an increase in the<a href="https://solaci.org/en/2022/05/05/prophylactic-rivaroxaban-therapy-for-left-ventricular-thrombus-after-st-segment-elevation-acute-coronary-syndrome/" title="Read more" >...</a>
Acute Coronary Syndrome: What Is Safer, Antiaggregant Monotherapy or De-Escalation?
For several years it has been shown that 12-month dual antiplatelet therapy (DAPT) is mandatory for patients undergoing left main PCI for acute coronary syndrome (ACS). However, though this strategy does reduce thrombotic events and mortality, it also causes undesirable bleeding events followed by hospitalization and antiaggregation interruption for a period of time. A feasible<a href="https://solaci.org/en/2022/03/09/acute-coronary-syndrome-what-is-safer-antiaggregant-monotherapy-or-de-escalation/" title="Read more" >...</a>
IVUS in Acute Coronary Syndrome: A New Requirement?
The use of intravascular ultrasound (IVUS) has seen exponential growth across registries over the years, combined with mounting and increasingly robust evidence. The fact that it will enable us to characterize plaque morphology and extension prior the intervention, and even assess stent expansion post intervention, has turned it into a pillar of our efforts to<a href="https://solaci.org/en/2022/03/07/ivus-in-acute-coronary-syndrome-a-new-requirement/" title="Read more" >...</a>